What are we aiming for?
In the mammalian central nervous system (CNS), and particularly in the human CNS, traumatic, ischemic or inflammatory lesions are often followed by inefficient repair attempts leaving us with scars and diminished function, resulting in persistent and sometimes even progressive neurological deficits.
So far a central obstacle for progress in this area of research has been the complex biology underlying the body’s response to CNS injury: acute CNS damage – irrespective of its trigger – is followed by a multi-cellular response and interactions which involve different cell types including neurons, astrocytes, microglia, oligodendrocytes and their precursors, as well as infiltrating immune cells. This response also spans multiple scales and develops from the superficial tissue level into the cellular and subcellular levels. In addition to the multiple responses a CNS injury can provoke, the idea that response to injury is highly context-dependent (the same cellular response can be beneficial in one setting or disease stage, but detrimental in another) has further hindered scientific research in the field.
Therefore our TRR 274 researchers aim to expand our knowledge on the complex biology underlying recovery after CNS injury, with the long-term vision to foster clinical translation and to help regenerative medicine achieve its goal of allowing humans to more fully recover after CNS damage.
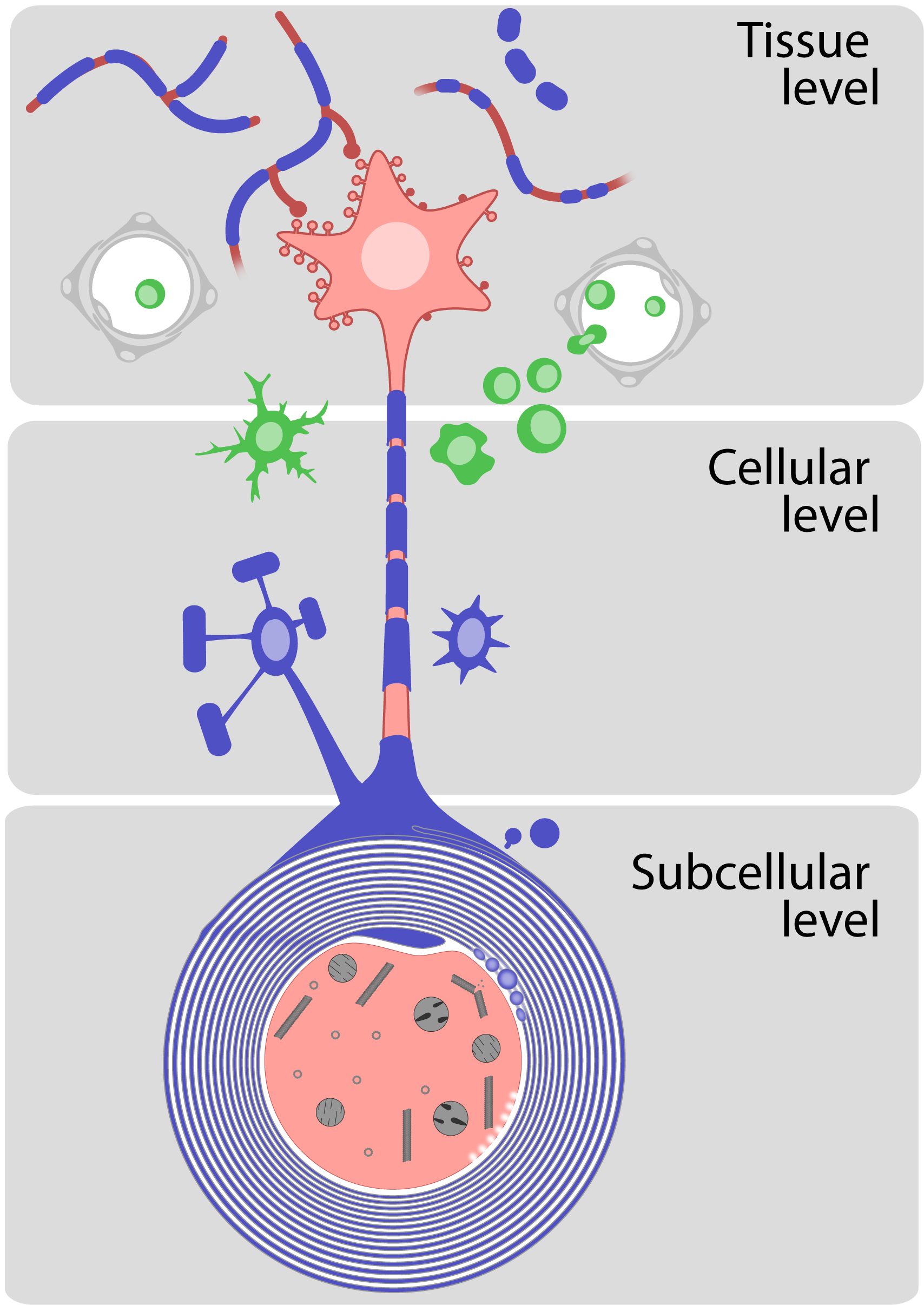
To achieve these goals, the our TRR 274 plans to understand the cellular activities and interactions underlying the mechanisms following CNS injury, at a multi-scale and -cellular level.
What is a checkpoint ?
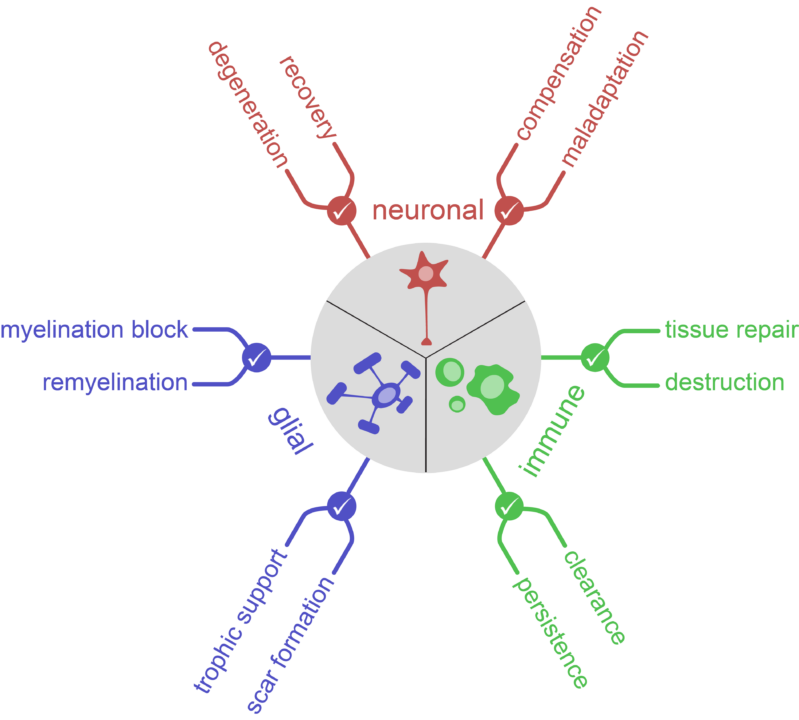
A checkpoint is a decision point, during the multi-cellular response to CNS injury, that defines lesion outcome. Much like a border where travellers are stopped for inspection, checkpoints in CNS recovery represent surveillance sites and mechanisms that monitor cellular or molecular responses that follow acute CNS injury. Such a checkpoint of either immune, glial or neuronal origin can – for example – be a molecular signal, a cellular surveillance mechanism or a tissue entry-exit site. A checkpoint, that is embedded in a cascade of events set off by an injury to the CNS, is a crucial step towards understanding whether the CNS will be able to recover from said injury or will succumb to it. By investigating such checkpoints, our goal is to obtain a comprehensive understanding of the endogenous determinants and mechanisms of CNS repair.
Innovation and Added Value
After several decades dominated by reductionist approaches, it is becoming increasingly clear that further progress on the biology of CNS recovery requires a novel, multi-disciplinary approach that integrates neuronal, glial and immune biology. In our view, only by systematically employing such an integrative approach can we fully understand the temporal and spatial dynamics of immune, glial and neuronal responses in CNS lesions that determine their outcome. Our TRR 274 gathers and connects researchers with diverse sets of scientific and technological expertise, from the field of immunology, neurobiology and glial biology. In order for us to uncover the crucial checkpoints of CNS recovery, we have established different inflammatory, traumatic, metabolic and vascular models of acute CNS damage, and the application of advanced imaging tools, „omics“-based methods as well as genetic approaches (including single cell RNA-Seq and cell-type-specific CRISPR/Cas9) at our three TRR 274 sites.
To further facilitate exchange of ideas and techniques between members of our TRR 274, all projects are integrated into a network of collaborations and some projects are even proposed as tandem projects, with 2 or more PIs. This will bring together scientists from different universities and research institutions with immune, neuronal and glial know-how and with basic or clinical background (bridging biology to medicine). Our common aim – to identify checkpoints of recovery – ties our TRR 274 together as a whole.
To achieve our goals we have three research areas, defined by the cellular location of their checkpoints:
Research Areas
The sequence of immune responses in injured CNS tissue, their duration and the composition of inflammatory infiltrates all vary depending on the type of injury, the site of the damage, environmental factors (e.g. microbiome, nutrition) and the genetic background. Nevertheless, there are certain common “ground rules”. Injury to the CNS triggers innate immune cell activation often underpinned by responses of the adaptive immune system. Microglia are the first to respond by proliferating and migrating to the area of injury, followed by neutrophils, monocyte-derived macrophages and lymphocytes. The cellular response after injury is normally modular in nature, occurring in distinct phases – starting with cell activation, followed by phenotype adaptation and ending with the resolution of the response. While immune cells play an important role in tissue repair (e.g. by phagocytosing debris and producing pro-regenerative factors), maladaptive immune reactions can lead to chronic or uncontrolled inflammation, in which persistent inflammation causes tissue damage. Here we want to understand the “ground rules” that initiate, sustain and terminate immune responses in the injured CNS. This will help us determine how the above-mentioned variations can be explained and – a prerequisite for future regulatory interventions – what significance these varying immune responses have for the integrity and function of nervous tissue. Based on these insights we want to identify the immunological checkpoints that govern the balance of the beneficial and harmful effects of the inflammatory reaction to CNS injury.
Glia, in particular astrocytes and oligodendrocyte precursor cells, are highly dynamic cells that quickly respond to CNS injury. Such responses include the upregulation of certain paracrine and autocrine growth and neurotrophic factors, as well as the secretion of pro- and anti-inflammatory cytokines and chemokines. These factors are not only responsible for initiating repair, for example by activating and recruiting oligodendrocyte precursor cells, but also for forming a barrier around the lesion site, a process referred to as reactive gliosis. Orchestrating these actions of glia to CNS injury is crucial to optimal recovery. Here, we want to understand how these activities are coordinated to allow regeneration to occur. In addition, glia and immune cells are highly intertwined and their inter-cellular signalling can result both in beneficial and harmful outcomes. For example, a subtype of reactive and neurotoxic astrocytes is induced by classically activated neuroinflammatory microglia, whereas regulatory T cells have been shown to directly promote oligodendrocyte differentiation and myelination. Thus we want to reveal the moleculare signals that mediate this multi-cellular communication and thereby identify the glial checkpoints that regulate protective actions of glial cells in the damaged CNS environment.
In general, neurons fail to regenerate spontaneously following injury, an outcome that is at least in part determined by inhibitory cues provided by the environment of the lesion site. Whereas regeneration is defined as the process of renewal and rebuilding of lost structures, repair is the process that stops further damage to the cell or tissue and aims to compensate for structural damage. Repair is just as important as regeneration, because CNS injury initially causes extensive irreversible neuronal damage that is subsequently amplified by the opening of the blood-brain-barrier and the local oedema. Understanding how cells such as neurons heal ruptured cellular structures and re-establish their glial support is crucial for the development of strategies that limit the spread of tissue damage in the CNS. Furthermore it is becoming increasingly clear that functional and structural adaptations of neuronal connectivity play a crucial role for neurological recovery after CNS injury and represent attractive new targets for restorative therapies. This is also a critical aspect of neuronal replacement therapies, as functional benefits also depend on the appropriate integration of transplanted neurons into pre-existing circuitry. Here we want to define the neuronal checkpoints that determine neuronal repair and rewiring on a molecular, cellular and network level and understand how local interactions with glial and immune cells shape the execution of these processes.
In addition to our 3 specialized research areas our TRR 274 has also established two service projects, that focus on providing methodological support, access to equipment, knowledge and expertise on cutting-edge bioimaging as well as “omics” technologies and techniques. The Bioimaging platform (Z01) allows each TRR 274 project to take advantage of various intra-vital, ultrastructural and nanoscopic imaging techniques at our 3 sites, aiming to dissect and observe processes on a cellular and even molecular level within each checkpoint of CNS damage/recovery. The Genomics and Bioinformatics Platform (Z02) centralizes and integrates, as the name hints, its expertise in high-throughput “-omics” techniques, as well as computational analysis of the resulting “big data” for all TRR 274 projects. As such, scientists are able to perform and utilize genomic methods, which amongst others include different bulk genomic analysis and single-cell methods and profit from the development of a standardized and centralized sequencing library for all projects. Furthermore, Z02 will offer transcriptomic, proteomic as well as lipidomic techniques to the consortium. The transfer and exchange of data and protocols within and throughout both platforms and TRR 274 projects is a key feature or our service projects and aims to guarantee comparability and reproducibility of results within our consortium, and thus to strengthen the significance of our findings as a whole.





